Sunday, February 2, 2025
How to Heal a Single Spot of Gum Pain with Healing Herbs

Soothing Sore Gums Naturally: A Herbal Approach
Experiencing a nagging spot of gum pain? Before rushing to the pharmacy, consider the soothing power of nature. Many readily available herbs possess anti-inflammatory and antiseptic properties that can effectively address minor gum irritations. This article explores several herbal remedies you can use to tackle that pesky gum pain, offering a gentler, natural alternative to over-the-counter medications. Remember, while these remedies can be very helpful for minor issues, persistent or severe gum pain always requires professional dental care.
Understanding the Source of Your Gum Pain
Before diving into herbal remedies, it's crucial to understand the potential cause of your gum pain. A single sore spot could indicate a variety of issues, from a minor irritation caused by food particles or a hard toothbrush bristle to something more serious, such as gingivitis or a developing infection. Identifying the underlying cause will help you determine the most appropriate course of action. If you suspect a more significant problem, schedule a visit with your dentist immediately. This article focuses on addressing minor gum irritations only.
Herbal Remedies for Gum Pain Relief
Several herbs possess powerful anti-inflammatory and antibacterial properties, making them effective in soothing irritated gums. Always use these remedies in moderation and discontinue use if you experience any adverse reactions.
Myrrh: A Powerful Antiseptic
Myrrh, a fragrant resin, has been used for centuries for its medicinal properties. Its antiseptic and anti-inflammatory actions can effectively combat infection and reduce swelling. You can use myrrh in a couple of ways: Create a rinse by mixing a small amount of myrrh tincture with warm water and gently swish it around the affected area for 30-60 seconds before spitting it out. Alternatively, you can find myrrh-infused toothpastes or mouthwashes at health food stores.
Chamomile: A Soothing Soother
Known for its calming effects, chamomile also boasts significant anti-inflammatory properties. Brew a strong chamomile tea bag in warm water, let it cool slightly, and then apply it directly to the affected gum using a clean cotton swab or gauze pad. Hold it in place for several minutes, repeating as needed throughout the day. The gentle warmth and chamomile's active compounds will work together to reduce pain and inflammation.
Sage: A Natural Antibacterial Agent
Sage, a culinary herb with many medicinal uses, contains antibacterial and anti-inflammatory compounds. Similar to chamomile, you can prepare a strong sage tea and use a cotton swab to apply it directly to the sore gum. Alternatively, you can rinse your mouth with cooled sage tea, allowing the beneficial compounds to come into direct contact with the irritated area.
Additional Tips for Gum Health
While herbal remedies can offer relief from minor gum irritation, maintaining good oral hygiene is paramount for preventing future issues. Here are some essential tips:
- Brush your teeth twice daily with a soft-bristled toothbrush.
- Floss daily to remove food particles and plaque from between your teeth.
- Use a fluoride mouthwash to further strengthen your enamel and protect against bacteria.
- Maintain a balanced diet, limiting sugary and acidic foods and drinks.
- Visit your dentist regularly for professional cleanings and checkups.
Remember, these herbal remedies are meant to complement, not replace, professional dental care. If your gum pain persists or worsens, schedule an appointment with your dentist immediately for proper diagnosis and treatment.
Best Probiotics for Gum Disease Prevention and Teeth Whitening Power
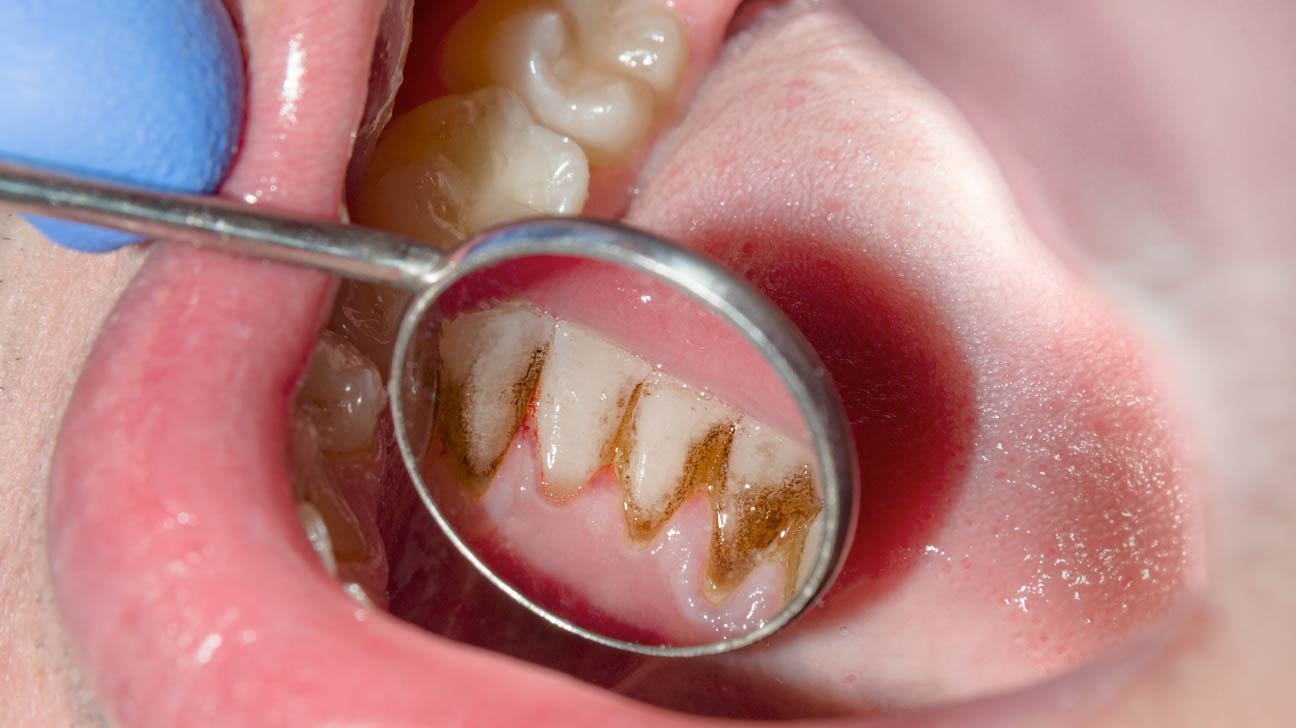
Unlocking a Healthier Smile: Probiotics for Gum Disease Prevention and Teeth Whitening
A dazzling smile isn't just about aesthetics; it's a reflection of overall oral health. While diligent brushing and flossing form the cornerstone of good oral hygiene, emerging research highlights the significant role probiotics play in preventing gum disease and even contributing to teeth whitening. This article explores the fascinating connection between probiotics and oral health, empowering you to make informed choices for a brighter, healthier smile.
The Gut-Mouth Connection: Understanding the Role of Probiotics
The relationship between your gut and oral health might seem surprising, but the two are intricately linked. Your gut microbiome, a complex ecosystem of bacteria, influences various aspects of your well-being, including immune function. A balanced gut microbiome supports a robust immune system, better equipped to fight off the bacteria responsible for gum disease (gingivitis and periodontitis). Probiotics, beneficial bacteria found in certain foods and supplements, help maintain this balance. By introducing beneficial bacteria into your gut, you indirectly strengthen your body's defense against oral pathogens.
Probiotics for Gum Disease Prevention: A Closer Look
Studies suggest certain probiotic strains effectively combat gum disease. These beneficial bacteria work in several ways: They compete with harmful bacteria for space and resources, reducing their population. They also produce substances that inhibit the growth of harmful bacteria, and even strengthen the integrity of your gums, making them more resistant to infection. Specific strains like Lactobacillus and Bifidobacterium species show promise in clinical trials, demonstrating a reduction in inflammation and bleeding gums associated with gingivitis. It's important to note that while research is promising, more large-scale studies are needed to definitively establish the efficacy of probiotics in preventing gum disease.
Choosing the Right Probiotic Supplement
Navigating the world of probiotic supplements can feel overwhelming. Look for supplements that specifically mention strains shown to benefit oral health, such as Lactobacillus rhamnosus GG, Lactobacillus reuteri, and certain Bifidobacterium strains. Check the label for the colony-forming units (CFUs), indicating the number of live bacteria in each dose. Higher CFUs generally translate to a greater potential benefit, but always follow the recommended dosage. Finally, choose reputable brands that ensure the quality and viability of their probiotic strains.
The Surprising Link Between Probiotics and Teeth Whitening
While the primary focus on probiotics is gum health, some indirect benefits contribute to whiter teeth. By reducing inflammation and gum disease, probiotics create a healthier environment in the mouth. Reduced gum inflammation minimizes discoloration around the gum line, leading to a visibly brighter smile. Furthermore, a healthy microbiome might indirectly influence the production of substances that contribute to plaque buildup, a major cause of tooth discoloration. While probiotics aren't a substitute for professional teeth whitening, they can contribute to a brighter smile as part of a comprehensive oral health routine.
Maintaining Optimal Oral Health: A Holistic Approach
Probiotics are a valuable addition to your oral health arsenal, but they shouldn't replace essential practices like:
- Brushing twice daily with fluoride toothpaste.
- Flossing daily to remove plaque and food particles.
- Regular dental checkups and cleanings.
- A healthy diet low in sugary and acidic foods and drinks.
Disclaimer: This information is for educational purposes only and should not be considered medical advice. Consult with your dentist or healthcare provider before starting any new supplement regimen, especially if you have pre-existing health conditions.
Prevent Plaque Buildup Naturally with Probiotics

Preventing Plaque Buildup Naturally with Probiotics: A Comprehensive Review
Dental plaque, a biofilm composed of bacteria, is the primary etiological factor in various oral diseases, including gingivitis, periodontitis, and caries. Traditional approaches to plaque control predominantly focus on mechanical methods such as brushing and flossing, supplemented by chemical agents like fluoride and antimicrobial mouthwashes. However, an emerging area of research explores the potential of probiotics as a natural and complementary strategy for preventing plaque accumulation and promoting oral health.
The Role of Oral Microbiota in Plaque Formation
The oral cavity harbors a complex and diverse microbial community, often referred to as the oral microbiota. This intricate ecosystem comprises hundreds of bacterial species, along with archaea, fungi, and viruses. Under normal circumstances, this microbiota exists in a state of relative equilibrium, maintaining a balance that prevents disease. However, disruptions to this balance, known as dysbiosis, can lead to the overgrowth of specific pathogenic bacteria, contributing significantly to plaque formation and the subsequent development of oral diseases.
The Keystone Pathogen Hypothesis
The keystone pathogen hypothesis suggests that certain bacteria, even if present in low abundance, can disproportionately influence the composition and function of the entire oral microbiota. Porphyromonas gingivalis, a Gram-negative anaerobe, is a prime example of a keystone pathogen strongly implicated in periodontitis. This bacterium produces various virulence factors, including gingipains, which degrade host tissues and modulate the immune response, facilitating the expansion of other pathogenic bacteria and the progression of disease.
The Influence of Dietary Factors
Dietary habits significantly impact the composition and activity of the oral microbiota. A diet high in refined sugars and processed carbohydrates provides a readily available energy source for plaque-forming bacteria, promoting their proliferation and exacerbating plaque accumulation. Conversely, a diet rich in fruits, vegetables, and fiber can contribute to a more balanced and resilient oral microbiota, potentially reducing the risk of plaque-related diseases.
Probiotics: A Novel Approach to Plaque Control
Probiotics, defined as live microorganisms that confer a health benefit on the host when administered in adequate amounts, have emerged as a promising alternative or complementary strategy for preventing plaque accumulation. The mechanism by which probiotics exert their beneficial effects is multifaceted and involves various interactions with the oral microbiota and the host immune system.
Mechanisms of Action
The beneficial effects of probiotics in preventing plaque buildup can be attributed to several mechanisms:
- Competition for Adhesion Sites: Probiotic bacteria can compete with pathogenic bacteria for binding sites on the tooth surface and salivary pellicle, hindering the colonization and growth of plaque-forming species.
- Production of Antimicrobial Substances: Some probiotic strains produce bacteriocins, hydrogen peroxide, and other antimicrobial compounds that inhibit the growth of pathogenic bacteria, reducing the overall bacterial load in the oral cavity.
- Modulation of the Immune Response: Probiotics can modulate the host immune response by stimulating the production of anti-inflammatory cytokines and reducing the inflammatory response associated with plaque-induced gingivitis and periodontitis.
- Enhancement of Salivary Flow: Some studies suggest that certain probiotics may stimulate salivary secretion, which plays a crucial role in clearing bacteria from the oral cavity and maintaining oral hygiene.
- Regulation of pH: Probiotics can contribute to maintaining a neutral oral pH, preventing the acidification associated with carbohydrate metabolism by pathogenic bacteria. This prevents demineralization of tooth enamel and reduces caries risk.
Probiotic Strains with Potential Anti-Plaque Activity
Several probiotic strains have shown promising results in preclinical and clinical studies for their ability to reduce plaque accumulation and improve oral health parameters. These include, but are not limited to:
- Lactobacillus reuteri
- Lactobacillus rhamnosus
- Streptococcus salivarius K12
- Weissella cibaria
The specific mechanisms of action and efficacy can vary among different probiotic strains, highlighting the importance of selecting appropriate strains based on their documented effects on the oral microbiota.
Clinical Evidence and Considerations
While the preclinical data supporting the use of probiotics for plaque control is encouraging, the clinical evidence remains somewhat limited. Many studies have demonstrated a reduction in plaque scores and gingival inflammation following probiotic intervention. However, the magnitude of the effect and the long-term sustainability of the benefits require further investigation. The variability in study designs, probiotic strains used, and outcome measures makes it challenging to draw definitive conclusions across all studies.
Challenges and Future Directions
Despite the promising potential of probiotics, several challenges need to be addressed to fully realize their clinical application in plaque prevention:
- Strain Specificity: The efficacy of probiotics is strain-specific. Not all probiotic strains are equally effective in reducing plaque accumulation. More research is needed to identify the most effective strains for targeting specific oral pathogens.
- Dosage and Delivery Methods: Optimizing the dosage and delivery method of probiotics is crucial to ensure their effectiveness. Different delivery systems, including lozenges, chewing gums, and mouthwashes, are being explored.
- Long-term Efficacy: Long-term studies are needed to evaluate the long-term efficacy and safety of probiotic interventions for plaque control. The sustainability of the beneficial effects after discontinuation of probiotic supplementation also requires further investigation.
- Individual Variability: The response to probiotic interventions can vary among individuals due to differences in their oral microbiota, dietary habits, and overall health status.
Future research should focus on identifying optimal probiotic strains, developing effective delivery systems, and conducting large-scale, randomized controlled trials to validate the clinical efficacy and safety of probiotic interventions for plaque control. Personalized approaches, considering individual differences in the oral microbiota, may also enhance the effectiveness of probiotic therapies.
Conclusion
Probiotics offer a promising natural approach to complement traditional methods for preventing plaque buildup and promoting oral health. While the clinical evidence is still evolving, the mechanisms by which probiotics exert their beneficial effects are well-established, including competition for adhesion sites, production of antimicrobial substances, and modulation of the immune response. Further research is needed to optimize probiotic formulations and delivery methods, ensuring their widespread and effective application in preventing plaque-associated oral diseases. The integration of probiotics into comprehensive oral hygiene strategies may contribute to improved oral health outcomes for individuals worldwide. However, it's crucial to remember that probiotics should be viewed as a complementary approach, not a replacement for regular brushing, flossing, and professional dental care.
The Benefits of Taking Collagen for Gum Recession
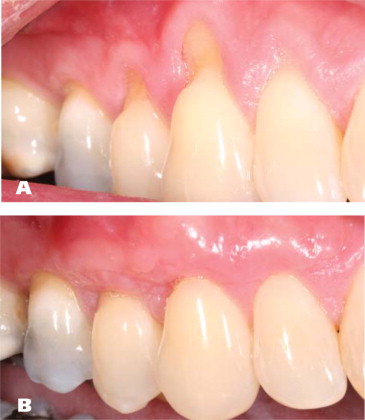
Reversing Gum Recession: Exploring the Potential Benefits of Collagen
Gum recession, the gradual pulling back of gums from the teeth, is a prevalent dental issue affecting millions. It exposes the tooth roots, making them vulnerable to sensitivity, decay, and even tooth loss. While traditional treatments exist, many individuals are exploring alternative approaches, including collagen supplementation. This article delves into the potential benefits of taking collagen for gum recession, examining the scientific evidence and highlighting its role in promoting gum health.
Understanding Gum Recession and its Causes
Gum recession stems from a variety of factors. Aggressive brushing techniques can wear away gum tissue over time. Periodontal disease, a bacterial infection affecting the gums and supporting bone structures, is a major culprit, causing inflammation and tissue breakdown. Genetics play a significant role; some individuals are simply predisposed to receding gums. Additionally, grinding or clenching teeth (bruxism) exerts undue pressure on the gums, contributing to recession. Understanding these causes is crucial in adopting preventative measures and exploring appropriate treatments.
Collagen's Role in Gum Health
Collagen is the most abundant protein in the human body, forming the structural framework of connective tissues, including gums. It provides strength, elasticity, and resilience. As we age, our natural collagen production diminishes, leading to a decline in tissue integrity and increased susceptibility to gum recession. Supplementation with collagen aims to replenish this deficit, bolstering gum tissue and promoting healing. Type I collagen, specifically, is critical for the structure of gums and periodontal ligaments, making it a primary focus in research and supplementation.
How Collagen Might Help Reverse Gum Recession
While definitive conclusions require further research, several mechanisms suggest collagen's potential benefit:
- Increased Tissue Regeneration: Collagen provides the building blocks for new tissue growth, potentially aiding in the regeneration of lost gum tissue.
- Reduced Inflammation: Some studies suggest collagen may possess anti-inflammatory properties, helping to combat the inflammation associated with gum disease and recession.
- Improved Gum Strength and Elasticity: Increased collagen levels may strengthen and increase the elasticity of gum tissue, making it more resistant to further recession.
It's important to note that collagen supplementation is not a standalone solution. It should be considered a complementary approach alongside proper oral hygiene and professional dental care.
Choosing a Collagen Supplement and Considerations
The market offers various collagen supplements, including hydrolyzed collagen peptides, which are readily absorbed by the body. When choosing a supplement, consider factors such as purity, source (e.g., bovine, marine), and dosage. Always consult with your dentist or physician before starting any new supplement regimen, particularly if you have pre-existing health conditions or are taking other medications. They can help determine the appropriate dosage and assess potential interactions.
Conclusion: A Promising Complementary Approach
Collagen supplementation shows promise as a complementary approach to managing and potentially reversing gum recession. While more research is needed to solidify its efficacy, the potential benefits related to tissue regeneration, inflammation reduction, and improved gum strength warrant further investigation. Remember, a holistic approach combining proper oral hygiene, professional dental care, and potentially collagen supplementation offers the best chance for maintaining healthy gums and preventing further recession.
Natural Ways to Soothe Sensitive Gums

Natural Ways to Soothe Sensitive Gums
Sensitive gums, characterized by discomfort, pain, and bleeding upon brushing or flossing, can significantly impact oral health and overall well-being. While professional dental care is crucial for addressing underlying issues, various natural remedies can effectively soothe sensitive gums and promote healing. This comprehensive guide explores a range of natural approaches to alleviate gum sensitivity, emphasizing the importance of a holistic approach to oral hygiene.
Understanding Gum Sensitivity
Gum sensitivity arises from various factors, including gum recession, periodontal disease (gingivitis and periodontitis), improper brushing techniques, aggressive flossing, acidic foods and beverages, hormonal changes, certain medications, and even mouth breathing. Receding gums expose the dentin, the underlying layer of the tooth, which contains microscopic tubules leading to the pulp (the nerve). These tubules are sensitive to temperature changes, pressure, and even air, leading to discomfort. Periodontal disease, an infection of the gums, causes inflammation, swelling, and bleeding, all contributing to sensitivity. Therefore, addressing the underlying cause is essential for long-term relief.
Identifying the Root Cause
Before embarking on any treatment, it is crucial to identify the underlying cause of gum sensitivity. A thorough dental examination is paramount. Your dentist can assess the health of your gums, check for signs of periodontal disease, and evaluate your brushing technique. They can also rule out other contributing factors, such as bruxism (teeth grinding) or oral allergies. Self-diagnosis should be avoided; professional guidance ensures appropriate and effective treatment.
Natural Remedies for Sensitive Gums
Numerous natural remedies can provide effective relief from sensitive gums. These methods often work by reducing inflammation, promoting healing, and strengthening the gum tissue. However, it is important to remember that these remedies are complementary to, not a replacement for, professional dental care.
Saltwater Rinses
Saltwater rinses are a time-tested and readily available remedy for soothing irritated gums. The salt's antiseptic properties help reduce inflammation and kill bacteria, while the water gently cleanses the area. To prepare a saltwater rinse, dissolve 1/2 to 3/4 teaspoon of salt in a glass of warm water. Swish the solution gently around your mouth for 30-60 seconds, then spit it out. Repeat several times a day, especially after meals. Avoid gargling vigorously, as this can further irritate sensitive gums.
Aloe Vera
Aloe vera, known for its anti-inflammatory and wound-healing properties, can effectively soothe sensitive gums. Its gel can be applied directly to the affected areas. You can either use the gel directly from an aloe vera plant or opt for a commercially available aloe vera gel specifically formulated for oral use. Apply a small amount to the gums using a clean finger or cotton swab, gently massaging it in. This can be done several times a day for optimal results.
Hydrogen Peroxide Rinse
Hydrogen peroxide, a mild antiseptic, can help kill bacteria and reduce inflammation in the gums. However, it's crucial to use it correctly and at the appropriate dilution. Never use undiluted hydrogen peroxide. Mix equal parts of 3% hydrogen peroxide and water. Swish the solution around your mouth for 30 seconds, then rinse thoroughly with water. Repeat this process once or twice a day. Overuse can irritate the gums and damage the tooth enamel, so it's essential to follow the recommended dilution and frequency.
Clove Oil
Clove oil possesses potent antibacterial and anesthetic properties, making it an effective remedy for gum pain and sensitivity. It contains eugenol, a compound with analgesic and anti-inflammatory effects. Apply a small amount of clove oil directly to the affected area using a cotton swab. Use with caution, as clove oil can be irritating in high concentrations. Dilute it with a carrier oil like coconut oil if needed. It's best to test a small area first to check for any adverse reactions.
Tea Tree Oil
Tea tree oil, known for its antiseptic and anti-inflammatory properties, can also help soothe sensitive gums. Similar to clove oil, it should be used with caution and diluted. Mix a few drops of tea tree oil with a carrier oil like coconut oil. Apply a small amount to the affected areas using a cotton swab. Always perform a patch test before widespread application to assess any potential allergic reactions.
Other Natural Approaches
Beyond these specific remedies, adopting certain lifestyle changes can significantly contribute to gum health and reduce sensitivity. These include:
- Maintaining a healthy diet: A diet rich in fruits, vegetables, and whole grains provides essential nutrients for gum health.
- Quitting smoking: Smoking significantly increases the risk of periodontal disease and gum recession.
- Reducing stress: Chronic stress can negatively impact the immune system, making individuals more susceptible to gum disease.
- Improving brushing techniques: Gentle brushing with a soft-bristled toothbrush, using a fluoride toothpaste, and employing proper brushing techniques can minimize gum irritation.
- Regular flossing: Daily flossing helps remove plaque and food particles from between the teeth and prevents gum inflammation.
- Staying hydrated: Drinking plenty of water helps maintain oral hygiene and wash away food particles.
When to Seek Professional Help
While natural remedies can provide relief from mild gum sensitivity, it's crucial to seek professional dental care if symptoms persist or worsen. Persistent bleeding gums, severe pain, swelling, loose teeth, or any noticeable changes in gum appearance warrant immediate attention. A dentist can accurately diagnose the underlying cause of your gum sensitivity and provide appropriate treatment, which might include scaling and root planing (deep cleaning), antibiotic therapy, or surgical intervention in severe cases of periodontal disease.
In conclusion, while natural remedies offer a valuable approach to managing sensitive gums, they should be considered complementary to professional dental care. Maintaining excellent oral hygiene, adopting a healthy lifestyle, and seeking timely professional help when necessary are critical for ensuring optimal gum health and preventing serious complications. Remember that early intervention is key in addressing gum sensitivity and preserving your long-term oral well-being.
The Role of Oral Probiotics in Reducing Bad Bacteria in the Mouth

The Role of Oral Probiotics in Reducing Bad Bacteria in the Mouth
The oral cavity, while seemingly a simple space, is a complex ecosystem teeming with a diverse microbial community. This community, referred to as the oral microbiome, comprises a vast array of bacteria, fungi, viruses, and archaea. Maintaining a balanced oral microbiome is crucial for overall oral health, as an imbalance, or dysbiosis, can contribute to various pathologies. Emerging research highlights the potential of oral probiotics – live microorganisms that confer a health benefit on the host when administered in adequate amounts – in modulating the oral microbiome and reducing the prevalence of pathogenic bacteria associated with oral diseases.
Understanding the Oral Microbiome and Dysbiosis
The oral microbiome is remarkably dynamic, exhibiting significant inter-individual and intra-individual variability influenced by factors such as age, diet, hygiene practices, and systemic health conditions. A healthy oral microbiome is characterized by a stable composition and a predominance of commensal bacteria, which contribute to host defense mechanisms and maintain a protective barrier against pathogenic microorganisms. These commensal bacteria produce various antimicrobial substances, compete with pathogens for nutrients and binding sites, and modulate the host immune response to prevent excessive inflammation.
The Role of Pathogenic Bacteria
Conversely, an overgrowth of pathogenic bacteria, such as Streptococcus mutans (contributing significantly to dental caries), Porphyromonas gingivalis (a key player in periodontitis), and Aggregatibacter actinomycetemcomitans (associated with aggressive periodontitis), disrupts the delicate balance of the oral microbiome. This dysbiosis leads to an inflammatory response, tissue damage, and the development of various oral diseases. The unchecked proliferation of these bacteria often outpaces the host's defense mechanisms, resulting in the onset and progression of oral pathologies.
Factors Contributing to Oral Dysbiosis
Several factors can contribute to the disruption of the oral microbiome and the subsequent development of dysbiosis. These include:
- Poor oral hygiene: Inadequate brushing and flossing allow the accumulation of plaque, providing an ideal environment for the proliferation of pathogenic bacteria.
- Dietary habits: A diet high in refined sugars and carbohydrates provides readily available substrates for the growth of cariogenic bacteria, such as S. mutans.
- Systemic diseases: Conditions like diabetes and HIV can impair the immune system, making individuals more susceptible to oral infections.
- Smoking: Smoking alters the composition of the oral microbiome, increasing the risk of periodontal disease and oral cancer.
- Antibiotic use: Broad-spectrum antibiotics can disrupt the balance of the oral microbiome, leading to the overgrowth of resistant pathogens.
The Potential of Oral Probiotics
Oral probiotics offer a promising avenue for modulating the oral microbiome and combating oral diseases. By introducing beneficial bacteria into the oral cavity, probiotics can help restore the balance of the microbial community, thereby reducing the prevalence of pathogenic bacteria and mitigating the risk of oral diseases. The mechanisms by which oral probiotics exert their beneficial effects are multifaceted and include:
Mechanisms of Action
- Competitive exclusion: Probiotic bacteria compete with pathogens for nutrients and attachment sites on the tooth surface and oral mucosa, limiting the growth and colonization of harmful bacteria.
- Production of antimicrobial substances: Many probiotic strains produce bacteriocins, hydrogen peroxide, and organic acids, which inhibit the growth of pathogenic bacteria.
- Modulation of the host immune response: Probiotics can interact with the host immune system, stimulating the production of antimicrobial peptides and enhancing the overall immune defense against pathogens.
- Enhancement of the host's natural defenses: Some probiotics may reinforce the natural protective mechanisms of the host, such as saliva production and the integrity of the oral mucosa.
Specific Probiotic Strains and Their Applications
Numerous probiotic strains have demonstrated potential in reducing oral pathogens. Lactobacillus species, such as Lactobacillus rhamnosus GG and Lactobacillus salivarius, have been extensively studied for their efficacy in preventing and treating various oral diseases. Streptococcus salivarius K12 is another promising probiotic strain, known for its ability to inhibit the growth of S. mutans. These strains are often incorporated into various delivery systems, including chewing gums, lozenges, and mouthwashes, to ensure optimal colonization and efficacy.
Evidence from Clinical Studies
While the research on oral probiotics is still evolving, several clinical trials have shown promising results. Studies have reported significant reductions in plaque scores, gingivitis, and halitosis in individuals using oral probiotic products. Furthermore, some studies have demonstrated a decrease in the levels of pathogenic bacteria, such as S. mutans and P. gingivalis, in individuals supplemented with oral probiotics. However, it is important to note that the results vary depending on the probiotic strain, the dosage, the duration of treatment, and the study design. Further, large-scale, well-designed randomized controlled trials are necessary to confirm these findings and establish definitive guidelines for the clinical application of oral probiotics.
Challenges and Future Directions
Despite the promising potential of oral probiotics, several challenges remain. One major challenge lies in the delivery of live probiotic bacteria to the oral cavity in sufficient numbers and maintaining their viability during storage and administration. Furthermore, the optimal probiotic strain or combination of strains for specific oral diseases needs further investigation. Standardization of probiotic products is crucial to ensure quality control and consistent efficacy. Future research should focus on:
- Identifying novel probiotic strains with enhanced efficacy against specific oral pathogens.
- Developing innovative delivery systems to ensure optimal colonization and viability of probiotics in the oral cavity.
- Conducting large-scale, well-designed clinical trials to evaluate the long-term effects and safety of oral probiotics.
- Investigating the interactions between oral probiotics and other factors, such as diet, lifestyle, and systemic health conditions.
- Exploring the potential of combining oral probiotics with other therapeutic approaches, such as antimicrobial agents and periodontal surgery, to enhance treatment outcomes.
In conclusion, oral probiotics represent a promising approach to modulating the oral microbiome and reducing the prevalence of pathogenic bacteria associated with oral diseases. While further research is needed to fully elucidate their efficacy and to establish clear clinical guidelines, the available evidence suggests that oral probiotics could play a significant role in improving oral health and preventing oral diseases. Continued research and development in this field are crucial to fully harness the potential of oral probiotics for maintaining a healthy oral ecosystem.
Using Probiotics as a Natural Solution for Gum Health and Hygiene

Harnessing the Power of Probiotics for Optimal Gum Health
For centuries, humans have sought natural solutions for maintaining optimal health, and oral hygiene is no exception. While traditional methods remain important, exciting advancements in the field of probiotics are offering a compelling, natural approach to bolstering gum health and hygiene. This article explores the fascinating world of probiotics and their potential to revolutionize how we care for our gums, offering a powerful alternative or complement to conventional treatments.
Understanding the Oral Microbiome and its Impact on Gum Health
Your mouth teems with a complex ecosystem of microorganisms, collectively known as the oral microbiome. This diverse community includes bacteria, fungi, viruses, and archaea, all interacting in a delicate balance. A healthy oral microbiome contributes significantly to overall oral health, aiding in nutrient breakdown and protecting against harmful pathogens. However, an imbalance, or dysbiosis, can lead to various oral health problems, most notably gum disease (gingivitis and periodontitis). Harmful bacteria can proliferate, triggering inflammation, gum bleeding, and ultimately, potential tooth loss. This highlights the critical need for maintaining a balanced oral microbiome.
Probiotics: Nature's Tiny Helpers for Gum Health
Probiotics are live microorganisms, primarily bacteria, that when administered in adequate amounts, confer a health benefit on the host. These beneficial bacteria can help restore balance to the oral microbiome by competing with harmful bacteria for resources and space, thereby reducing their numbers and minimizing their negative impact. Furthermore, some probiotics produce substances that directly inhibit the growth of pathogenic bacteria, further strengthening the defense against gum disease.
Mechanisms of Action: How Probiotics Work Their Magic
The beneficial effects of probiotics on gum health manifest through several mechanisms:
- Competitive Exclusion: Probiotics occupy binding sites on the gum tissue and teeth, preventing harmful bacteria from attaching and colonizing.
- Production of Antimicrobial Substances: Certain probiotic strains produce substances like bacteriocins and hydrogen peroxide that directly kill or inhibit the growth of harmful bacteria.
- Immune Modulation: Probiotics can stimulate the immune system, enhancing the body's natural defenses against inflammation and infection in the gums.
- Reduced Inflammation: By counteracting the harmful effects of pathogenic bacteria, probiotics help reduce inflammation in the gum tissues, alleviating symptoms like bleeding and swelling.
Evidence-Based Support for Probiotic Use in Gum Health
While research is ongoing, several studies have demonstrated the potential benefits of probiotics in improving gum health. These studies show a reduction in gingival inflammation, bleeding, and plaque accumulation in individuals using probiotic-containing mouthwashes, gels, or supplements. However, it's crucial to note that the effectiveness of different probiotic strains varies, and more research is needed to establish optimal strains, dosages, and delivery methods for consistent and significant results. Always consult with your dentist or healthcare provider before starting any new supplement regimen.
Incorporating Probiotics into Your Gum Health Routine
Integrating probiotics into your oral hygiene routine can be achieved through various approaches. You can find probiotic-containing mouthwashes and toothpastes readily available at many health stores and pharmacies. Additionally, certain foods rich in probiotics, such as yogurt with live and active cultures, can contribute indirectly to a healthier oral microbiome. However, remember that the effectiveness of these products varies, and choosing products with scientifically proven strains is essential for optimal results. Regular brushing, flossing, and professional dental cleanings remain crucial components of a comprehensive oral hygiene regimen. Probiotics should be considered a complementary approach, not a replacement for these established practices.
In conclusion, probiotics offer a promising avenue for enhancing gum health and hygiene, providing a natural and complementary approach to maintaining a balanced oral microbiome. While further research is warranted to fully elucidate their potential, the existing evidence strongly suggests that these tiny allies can significantly contribute to a healthier, happier smile.